- What is Inflammatory Arthritis of the Hip?
- What Are Common Symptoms of Inflammatory Arthritis of the Hip?
- What Are the Common Causes and Risk Factors for Inflammatory Hip Arthritis?
- Diagnosis and Evaluation
- How Can Inflammatory Arthritis of the Hip Be Treated?
Managing arthritis of the hip can be challenging, but with the right treatment and care, it’s possible. Approximately 54 million adults in the United States are diagnosed with some form of arthritis, with a significant portion of these cases being inflammatory arthritis, according to the Arthritis Foundation.
What is Inflammatory Arthritis of the Hip?
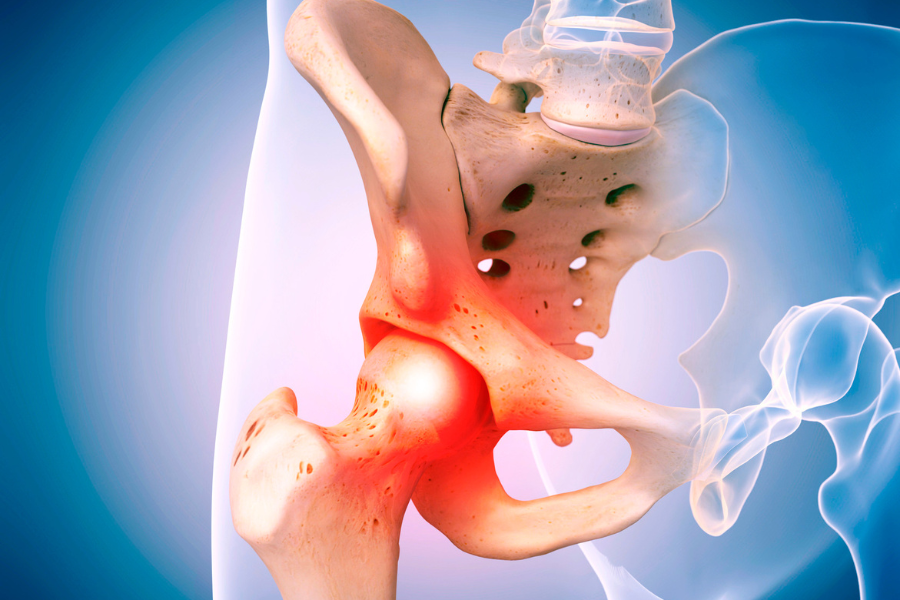 Inflammatory arthritis of the hip refers to a group of chronic joint disorders that primarily affect the hip joint and are characterized by inflammation, pain, and stiffness. These conditions are part of a larger category of autoimmune diseases known as inflammatory arthritis, which involves the immune system mistakenly attacking healthy joint tissues, leading to inflammation and joint damage.
Inflammatory arthritis of the hip refers to a group of chronic joint disorders that primarily affect the hip joint and are characterized by inflammation, pain, and stiffness. These conditions are part of a larger category of autoimmune diseases known as inflammatory arthritis, which involves the immune system mistakenly attacking healthy joint tissues, leading to inflammation and joint damage.
It’s important to differentiate between osteoarthritis and inflammatory arthritis because their causes and treatment approaches differ significantly. Osteoarthritis is primarily caused by joint wear and tear, while inflammatory arthritis is an autoimmune condition in which the body’s immune system attacks the joint lining. Differentiating between the two impacts the course of treatment and the outcome.
Common Types of Inflammatory Arthritis Affecting the Hip
Some of the common types of inflammatory arthritis that can affect the hip joint include:
- Rheumatoid Arthritis (RA): RA is an autoimmune disease where the immune system mistakenly attacks the synovium in various joints, including the hips. This can lead to inflammation, pain, joint damage, and deformity over time.
- Ankylosing Spondylitis (AS): AS primarily affects the spine but can also affect the hip joints. It is characterized by inflammation of the spine and sacroiliac joints (the joints connecting the spine to the pelvis).
- Psoriatic Arthritis: This form of arthritis occurs in some people with psoriasis, a skin condition. Psoriatic arthritis can affect multiple joints, including the hips, causing inflammation, pain, and damage.
- Juvenile Idiopathic Arthritis (JIA): JIA is a term used to describe various types of arthritis in children. Some forms of JIA can involve the hip joint and cause inflammation and joint problems.
- Reactive Arthritis: Reactive arthritis is triggered by an infection in another part of the body, such as the urinary or gastrointestinal tract. It can lead to inflammation in the joints, including the hips.
What are Common Symptoms of Inflammatory Arthritis of the Hip?
Inflammatory arthritis of the hip can occur with various symptoms, and the severity and progression of these symptoms can vary from person to person. Early signs and common symptoms of hip inflammatory arthritis may include:
- Joint Pain: Persistent and often deep pain in the hip joint is a hallmark symptom. The pain may be dull, aching, or sharp and can worsen with movement or weight-bearing activities.
- Stiffness: Hip joint stiffness, particularly in the morning or after periods of inactivity, is common. This stiffness can limit your ability to move the hip freely.
- Swelling: Inflammation in the hip joint can lead to localized swelling, which may cause visible enlargement of the joint.
- Warmth and Redness: Inflammation can cause the skin over the hip joint to become warm and red, particularly during flare-ups.
- Limited Range of Motion: Hip inflammatory arthritis can result in reduced flexibility and limited range of motion in the affected hip. You may have difficulty walking, bending, or lifting your leg.
- Fatigue: Chronic inflammation can lead to fatigue, affecting overall energy levels and quality of life.
- Pain in Other Joints: Some individuals with inflammatory arthritis may experience pain and swelling in other joints, such as the knees, shoulders, or wrists, as these conditions often affect multiple joints.
- Morning Stiffness: Many people with hip inflammatory arthritis experience stiffness in the hip joint, which is often more pronounced in the morning or after prolonged rest periods. This morning stiffness can last for 30 minutes or more.
- General Malaise: You may feel generally unwell, with symptoms such as fever and feeling sick.
It’s important to note that the symptoms of hip inflammatory arthritis can mimic those of other hip conditions, such as osteoarthritis or bursitis.
What Are the Common Causes and Risk Factors for Inflammatory Hip Arthritis?
 It can be challenging to prevent and intervene early in hip inflammatory arthritis without knowing its underlying causes and risk factors. Understandably, we know this can be frustrating and worrisome. Some possible causes and risk factors that researchers have identified include:
It can be challenging to prevent and intervene early in hip inflammatory arthritis without knowing its underlying causes and risk factors. Understandably, we know this can be frustrating and worrisome. Some possible causes and risk factors that researchers have identified include:
- Autoimmune Diseases: Rheumatoid arthritis, ankylosing spondylitis, and psoriatic arthritis can cause chronic inflammation and damage various body parts.
- Infections: The Hip joint can be affected by bacterial or viral infections leading to conditions.
- Genetics: A family history of autoimmune diseases increases the risk.
- Age and Gender: Some types are more common in certain age groups or genders.
- Hormones: Hormonal factors can influence specific types of arthritis.
- Environmental Factors: Smoking and other environmental factors can contribute.
- Obesity: Excess weight can stress the hip joints.
- Injury or Trauma: Past hip injuries or trauma may play a role.
- Other Health Conditions: Conditions like inflammatory bowel disease can increase the risk
Diagnosis and Evaluation
Diagnosing hip inflammatory arthritis requires a comprehensive evaluation. Our team at Louisville Hip & Knee Institute employs a range of diagnostic tools, including:
- History and Physical Examination: Assess symptoms and conduct a physical exam to check for joint inflammation and mobility issues.
- Blood Tests: Measuring markers like ESR, CRP, RF, and specific antibodies to detect inflammation and autoimmune factors.
- Imaging: X-rays, MRI, and ultrasound visualize joint damage, inflammation, and soft tissue involvement.
- Joint Aspiration: Collecting synovial fluid from the hip joint to confirm inflammation.
- Specialized Tests: Additional tests such as HLA typing or skin biopsies may be performed depending on the condition.
Early diagnosis is important for timely treatment and better outcomes in inflammatory hip arthritis.
How can Inflammatory Arthritis of the Hip be Treated?
 Treating and managing hip inflammatory arthritis aims to relieve pain, reduce inflammation, preserve joint function, and improve overall quality of life. Treatment options may include:
Treating and managing hip inflammatory arthritis aims to relieve pain, reduce inflammation, preserve joint function, and improve overall quality of life. Treatment options may include:
- Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs), disease-modifying antirheumatic drugs (DMARDs), and biologic agents can help control symptoms and slow disease progression.
- Physical Therapy: Targeted exercises and physical therapy can improve joint function, reduce pain, and enhance mobility.
- Lifestyle Modifications: Weight management and assistive devices may be recommended to reduce stress on the hip joint.
- Surgery: In severe cases of ineffective conservative treatments, surgical options like hip replacement may be considered.
Collaborating closely with your healthcare team to develop a personalized treatment plan that works for you is important.
Depending on your condition, the team may include rheumatologists, orthopaedic surgeons, physical therapists, and other specialists. Regular monitoring and adjusting your treatment plan may be necessary to manage the condition effectively and improve your hip’s function and overall quality of life.
Next Steps for Your Hip Arthritis
Inflammatory arthritis of the hip is a complex condition that can significantly impact your daily life. If you or a loved one is experiencing symptoms of hip inflammatory arthritis, don’t hesitate to schedule an appointment with us today. Our orthopaedic experts are here to provide the care and support you need to manage this condition effectively.

